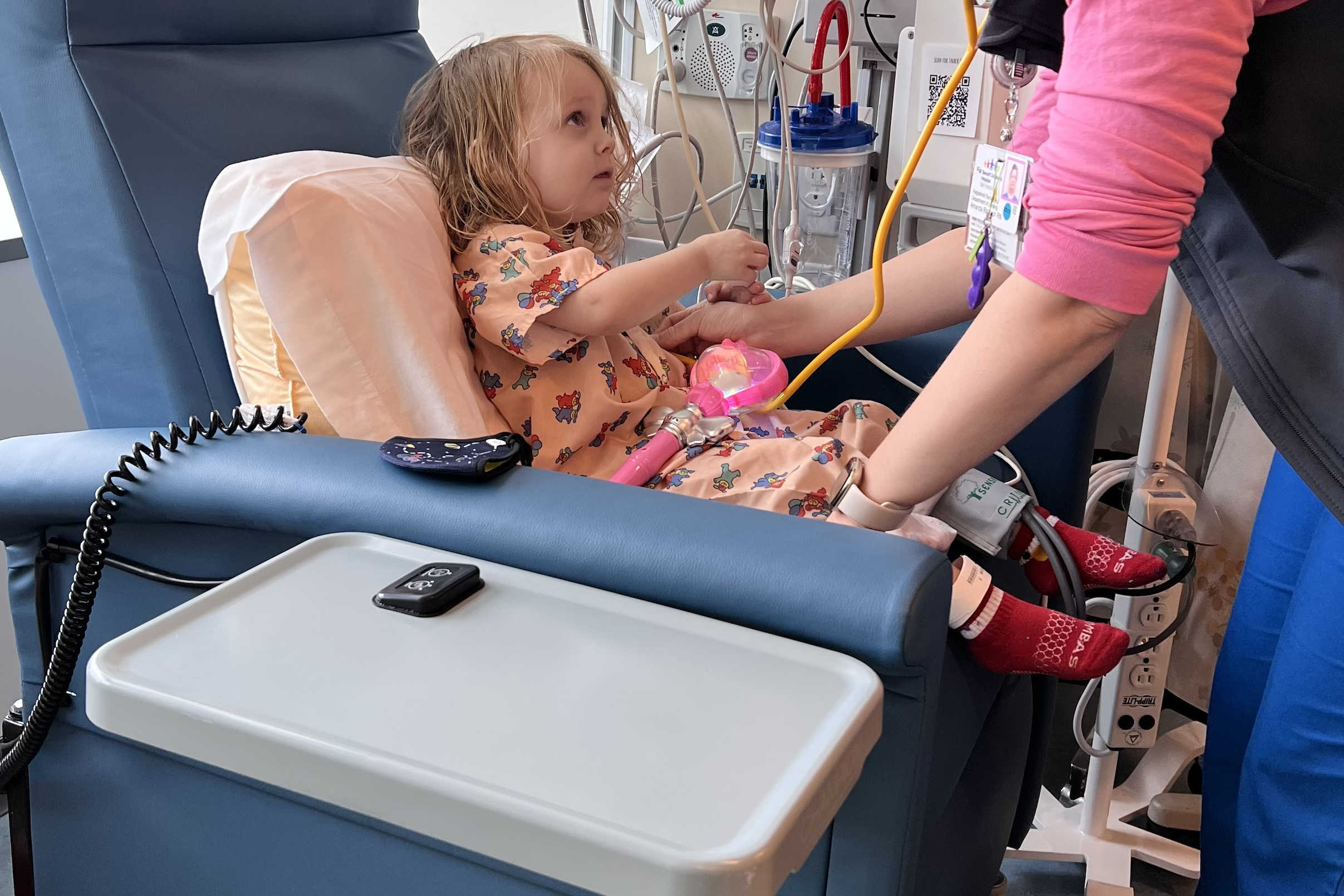
When Caitlin Bauer’s infant daughter Vivian needed food allergy tests, she took her to UCSF Medical Center in Mission Bay, the same place where the baby was delivered.
Three years and many tests later, Bauer loves her daughter’s allergist and the quality of care at UCSF. But she has come to despise the billing department.
Bauer says UCSF Health has repeatedly charged her too much or double-billed Vivian’s allergy tests. Often the largest expenses have been vague “facility fees” that leave Bauer on the hook for hundreds of dollars after insurance.
But unlike most patients, who simply accept the bill, Bauer has a superpower: “I have ADHD, and I’m just extremely interested in researching things,” she said.
Through her own research, Bauer has grown unusually skilled at navigating the Current Procedural Terminology, the arcane codes used by the medical profession to report services for billing. And she’s using that knowledge to fight back—often successfully—one bill at a time.
Bauer’s ability to navigate medical billing as a layperson may be unusual, but her predicament is not.
Some San Franciscans say that UCSF Health has hit them with huge, unexpected bills that just don’t make sense. They have found themselves torn between the University of California system’s superior medical care and the exorbitant prices.
Their experiences may become more common.
UCSF Health—already San Francisco’s largest hospital and second-largest employer—is poised to acquire two more local hospitals and several other medical facilities, increasing its foothold in local healthcare.
Experts say that is part of an ongoing national trend towards consolidation of medical centers that isn’t doing patients any favors.
“These are dominant, gorilla- or elephant-sized hospital systems,” said Daniel O’Neill, a former health policy fellow at the National Academy of Medicine. “And it has not improved healthcare and it has increased the cost of healthcare.”
For its part, UCSF places the blame for large bills on insurers.
“The amount patients pay for their health care–including their co-pay, deductible, and percentage of care costs–is determined by their health insurance company and individual health plan,” the university said in a statement to The Standard. “It is not controlled by UCSF Health or their care provider.”
Big Bills
It’s not just facility fees.
Bauer says that, in just over a year, she saw the prices of similarly coded allergy tests for her daughter more than double. And other patients have received charges that they say stretch believability.
When Tyler Hilligoss moved to the Bay Area from Minnesota two years ago, he knew he needed to find a new gastrointestinal doctor to manage his Crohn’s disease.
He turned to Reddit and other online forums for advice. Many people recommended UCSF.
In 2021, he had a new patient video visit with a UCSF GI specialist. Because Hilligoss was diagnosed over 20 years ago and his disease is in remission, the visit was largely a formality. It lasted no more than 10 minutes, he said.
But then, he told The Standard, he got the bill: over $1,100 for a visit the medical center claimed took 45 minutes. Only $200 was covered by insurance, even though UCSF was in network.
Are you a UCSF patient having difficulty understanding or paying bills? Email us at tips@sfstandard.com. You can also call us at 415-408-6000 or send us a text message at 415-408-6282.
“It seemed extraordinary because most of my visits—even my more detailed office visits—back in Minnesota were at most $400,” Hilligoss said. “And those sometimes included a blood draw as well.”
After Hilligoss inquired about the cost and the medical center’s claim that the consultation lasted 45 minutes, he says UCSF told him he was being billed both for the time the doctor spent with him and reviewing his medical file.
Even though he had doubts about that calculation, Hilligoss didn’t fight it.
“I’m fairly used to health care being awful in this country, so it’s just kind of another drop in the bucket on that,” he said. “I got off lucky because it could have been something that charged me $30,000 instead [when it] should have been $2,000 dollars.”
Another woman, who asked not to be named because she works in the UCSF system and fears retaliation, said she has found it difficult to avoid unexpected bills.
Following an annual wellness visit, which should have been fully covered by insurance as a preventative exam, she received bills for an office visit and bloodwork. The reason she was told: She had mentioned a new issue that wasn’t on her record. That led to the visit being coded differently.
When the woman called UCSF and explained the situation, the billing department agreed to recode the visit as an annual wellness visit, she said.
But after experiencing this billing issue several times, she now begins such visits with a script: “I’m here for my preventative exam, my annual exam, that’s covered by my insurance.”
“And I’ll just ask [the doctor] to be mindful of what she’s writing down,” she added.
UCSF did not comment on what is causing these patients to receive such large bills but attributed higher prices to the fact that it is an academic medical center providing highly specialized care.
“Patients who are referred to UCSF Medical Center typically have more acute conditions than those who seek care in a community hospital or clinic, even if the services might sound the same on the surface,” the university said in a statement. “The care provided to these patients may cost more than it would in a community setting due to the number of specialists involved and the level of multi-disciplinary or complex care they receive.”
‘Nothing Is Straightforward’
So what is going on in these situations? Experts say that facility fees and rising costs are a consequence of growing hospital consolidation. The issue is so common nationally that it recently was the subject of an op-ed in the New York Times.
But determining when a medical center can charge a facility fee is more complicated.
With Bauer’s permission, The Standard shared a 44-page dossier she had compiled about her UCSF bills with Susan Null, who co-owns medical billing and patient advocacy company Systemedic. Null reviewed the document, which included images of Bauer’s bills, screenshots of her online communications with UCSF, as well as her personal notes from her struggle to have UCSF bills overturned.
Although Null’s conclusions were far from definitive, they were instructive.
She said that while many of the charges appeared to be legitimate—i.e. the insurance company accepted them under its contract with UCSF—that didn’t necessarily make them reasonable.
But fully auditing the charges would require reading more documents, reviewing the actual itemized bills against the insurance company’s explanation of benefits, delving into Bauer’s insurance policy, having detailed conversations with UCSF and answering many more questions.
“Unfortunately, nothing in medical billing is straightforward,” Null said.
In the last few decades, the cost of running a medical practice has risen sharply. Small providers like individual doctor’s offices are being pushed out of the market or bought up by major medical centers, according to Null.
These medical centers become “a mammoth in terms of their negotiating power with an insurance company,” she said. They can charge insurers significantly more for the same medical services and procedures. And unlike an individual physician with his or her own practice, medical centers can charge for use of their facilities alongside regular doctor fees.
This is one of the factors driving big medical centers to purchase smaller practices: “It’s just another way for them to add on another layer of expense,” Null said.
According to Null, it is up to the insurer to decide whether the facility fee is legitimate. If the insurance company believes it is not, then they should fight it out with the hospital, she said.
But in Bauer’s experience, her insurance company wasn’t aware whether the charge was legitimate.
After investigating her bills, she concluded that UCSF was billing her incorrectly for her daughter’s oral food challenges—an allergy test that involves supervised and monitored consumption of a potential allergen.
When Bauer brought the issue to the attention of her insurer, they agreed and said UCSF was trying to present the test as an outpatient surgical facility, which meant she would be responsible for 20% of the cost under her plan. The insurer then asked UCSF to return their money and resubmit the claim.
Powerless Patients
To O’Neill, the former fellow at the National Academy of Medicine, these issues are reason enough to be worried about UCSF’s plan to acquire St. Mary’s Medical Center and Saint Francis Memorial, two hospitals operated by Dignity Health, and several other practices.
Today, there is robust evidence that hospital consolidation leads to higher prices. And a study by the Rand Corporation shows that all hospitals in San Francisco are already expensive, O’Neill said.
This contributes to situations like Hilligoss’s $1,100 video visit, which O’Neill described as “laughably overpriced” and “absurd.”
Moreover, in a world where pricey bills and unexpected charges are increasingly the reality, patients can do little to protect themselves. Even pushing back against big bills and contacting the state regulator, the Department of Managed Health Care, has limited effect.
“Until we decide at the national level, at the state level, to stop providers from abusing the system, we are not going to get change and patients will not be able to protect themselves,” he said.
He also disagrees with Null that private practices are no longer financially viable. Rather, he believes they are forced to compete with the deep pocketed medical centers when hiring.
“It’s a bit like a small tech company trying to compete with Google,” O’Neill said.
Short of implementing a public option for healthcare, he thinks the best thing policymakers can do to protect patients is to put a limit on all out-of-network charges from hospitals or health systems at or close to the rate that Medicare pays.
If implemented for health insurance plans sponsored by employers, this rule would tilt the bargaining dynamic, which currently benefits large medical providers, in favor of insurers and help drive down prices, O’Neill said.
But barring that change, patients need to do what they can to protect themselves. For Bauer, that means fighting the big bills.
For the past three years, she has gotten UCSF to overturn large fees. She kept fighting because she believed what the medical center was doing wasn’t right.
“I think about people who don’t have the money, they don’t have the resources, who don’t have insurance, and it just feels so wrong,” she said.
But even Bauer has limits. She said she and her daughter have now moved to a new clinic in Redwood City.